Horse fungus can occur at any time and almost anywhere on the horse’s body, legs, and hooves, causing issues that range in severity from relatively benign to life-threatening.
A couple of months ago, my 17-year-old Arab mare developed cracks and discoloration on one of her hind hooves. Horse fungus can be frightening when your horse catches it.
Is horse fungus contagious? There are four broad categories of horse fungus comprising over 50,000 species: Superficial Horse Fungus (Ringworm), Cutaneous Fungus, Subcutaneous Fungus, and Deep Mycoses. Three of the types of horse fungus are highly contagious. Horse fungus passes quickly between horses and can spread through a shared environment, grooming equipment, trailers, stables, and tact.
Let’s dive into understanding horse fungus and what you need to watch out for.

A closer inspection revealed some separation between the sole and the hoof wall and a retracted coronary band. My horse didn’t seem to be too concerned about the problem, showing no signs of discomfort or lameness, but I consulted my farrier and a few other experts anyway.
Initially, the consensus was that the cracking was due to a lack of biotin in my horse’s diet, but then my farrier came up with an alternative theory. According to him, the problem was a type of horse fungus that had flourished in the heavy dew and generally damp conditions of our South African summer.
This issue is just one of many types of horse fungus that can attack your horse’s skin, eyes, and hooves.
Signs of Horse Fungus
Each fungus has its unique identifiers, and another health issue can cause many symptoms of horse fungus. But, by understanding the common symptoms of horse fungus, you will be better prepared to respond to your horse’s needs and possibly save its life.
- Skin lesions
- Loss of appetite
- Rapid breathing
- Breathing Distress
- Skin sores with pus
- Cough
- Hemoptysis
- Weight loss
- Ulcerated skin
- Colic
- Lethargic
Most Common Types of Horse Fungus
There are four classes of horse fungus, each of which produces different symptoms. If your horse has trouble breathing, develops skin lesions and sores, loses patches of hair, or develops a cough, it may have a type of horse fungus.
Other symptoms include rashes, sores with pus, and unexplained colic. Have your horse diagnosed and checked for fungus. Fungus is a critical condition and should not be ignored.
Superficial Horse Fungus
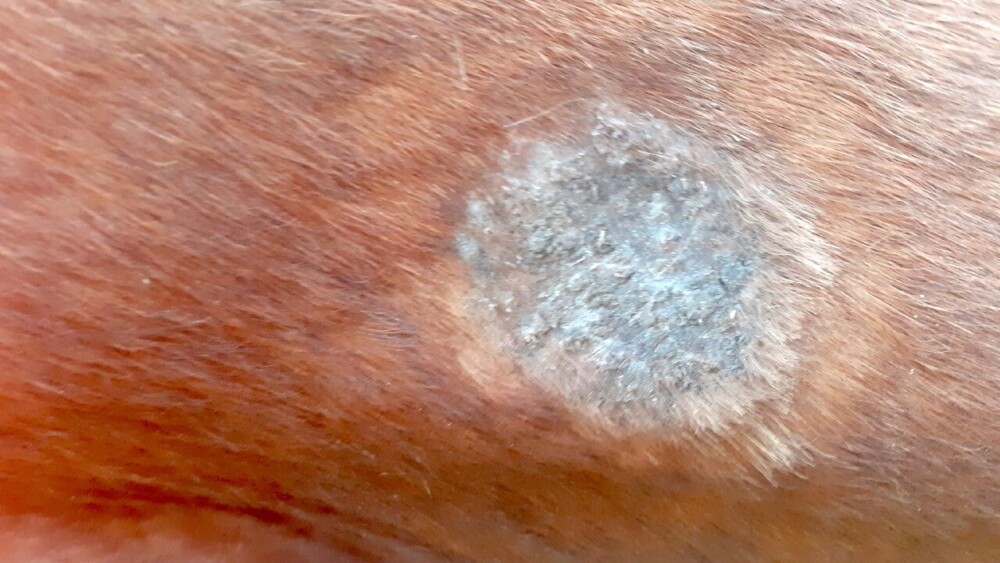
This class of fungal infection is generally benign but often highly contagious. The most common type of superficial mycosis is dermatophytosis, also known as ringworm or girth itch. These are usually relatively easy to identify due to the characteristic lesions on the horse’s skin.
A horse with ringworm will develop scaly patches of skin with the hair missing or broken off. The patches will be circular and bald. Usually, flaky patches show up around the saddle area and girth.
Ringworm is relatively easy to treat. But, it’s is highly contagious. The fungus can survive for months in contaminated equipment and clothing.
Cutaneous Fungus Diseases
While superficial horse fungus attacks only the skin, cutaneous fungus diseases affect both the skin and the hair. These are among the most common types of horse fungus and, like superficial mycoses, are caused by dermatophytes.
Infections of this nature cause skin lesions to those seen with ringworm. Without early diagnosis and treatment, cutaneous fungal infections can lead to more critical problems, including lethargy, loss of appetite, and colic.
Subcutaneous Horse Fungus
This class of fungus diseases infects the skin and the subcutaneous tissue. In severe cases, it may even move to the underlying tissues and organs. Early signs of a subcutaneous fungal infection include the appearance of nodular lesions at the contamination site.
Skin lesions may give off cream-colored pus that is blood-tinged. The pus usually doesn’t smell. Fortunately, most subcutaneous fungi are not contagious and respond well to treatment.
Deep Mycoses
Deep Mycoses is by far the most dangerous fungus. It usually affects the upper and lower respiratory tract. You may notice a difference in the way your horse breathes.
After the lungs are infected, the fungus often moves around the body and can quickly affect vital organs and the lymph nodes.
Deep Mycoses can be fatal. You must recognize the warning signs and seek an early diagnosis. With early diagnosis, your horse has a good chance of recovery.
The most common types of serious horse fungus include pneumocystis carinii and aspergillosis. The first causes respiratory problems and fever. Aspergillosis usually occurs in immune-suppressed horses and causes nasal discharge, drooping eyelids, and breathing difficulties.
Deep Mycoses are more challenging to diagnose and require immediate veterinary intervention. To determine if your horse has a deep fungal infection, a vet would need to take x-rays and perform an endoscopy to examine the guttural pouch. While treatments are usually effective, if the fungus has caused nerve damage, the horse may not make a full recovery.

What’s the Best Treatment For Horse Fungus?
It’s possible to treat most superficial horse fungi effectively with a topical, anti-fungal ointment or spray. You can even use an over-the-counter human treatment for an athlete’s foot.
First, treat superficial mycoses, clean the lesions and the areas around them thoroughly with antibacterial soap, then apply your chosen anti-fungal cream to the lesions. For the first seven days, this should be done daily, after which you can drop it down to a couple of times a week.
To prevent the horse fungus from spreading to other animals and humans, make sure you wash your hands thoroughly after treating the problem and wash all your grooming equipment, stable, head collars, and tack every day with antiseptic.
Fungus thrives in dark, damp conditions. So, an infected horse will benefit from exposure to air and sun. Where possible, avoid rugging and give your horse as much turnout time as possible.
Cutaneous and subcutaneous fungal infections also respond well to topical medications and benefit from exposure to air and sun. In some instances, you may need to use oral medication in conjunction with a topical treatment to kill the fungus and facilitate the healing process.
More severe cases of horse fungus may require a course of corticosteroids or even surgery to remove lesions and fungal granulomas. Fungus can hide in the nasal passages.
Natural Remedies for Horse Fungus
If, like me, you prefer a more natural approach, you can use apple cider vinegar instead of an anti-fungal ointment. Apple cider vinegar has strong anti-fungal properties and can help treat ringworm and other similar horse funguses if applied topically. I used it to treat my horse’s hoof fungus and got great results from applying it topically three times a day.
Other natural remedies include:
- Garlic – make a paste by crushing up garlic cloves and combining them with coconut or olive oil, then apply the paste to the affected areas.
- Aloe vera – this succulent plant has anti-fungal, antibacterial, and antiviral properties, making it effective in treating superficial horse fungus. Apply the gel to the lesions three or four times a day.
- Turmeric – this potent anti-inflammatory also has “extensive antimicrobial abilities,” which make it an effective treatment for ringworm and other similar horse fungi. It can be added to your horse’s food and made into a paste for topical application.

The Problems Of Self-Diagnosing Horse Fungus: A Case Study
Even equipped with the information above, self-diagnosing a horse fungus can endanger your horse’s life.
An 11-year-old Saddle horse in New Zealand developed what appeared to be an allergic reaction following an operation on his splint bone. Nodules and lesions appeared on the horse’s neck a week after the surgery. The horse’s owner assumed this was an allergic reaction and treated him with corticosteroids.
The horse showed no improvement and developed further complications, including loss of appetite, weight loss, and colic. Blood, hair, and skin samples taken by the consulting vet ruled out an allergic reaction and identified yeast-like structures indicative of a horse fungus known as Geotrichum candidum.
The horse was subsequently treated with both “an antifungal solution and antioxidants,” making a complete recovery. In a report on the case, however, the authors suggested that “the early corticosteroid treatment may have impaired the immune system of this horse, making the horse susceptible to contracting a fungal infection.”
The study team concluded that any owner suspecting horse fungus should call a vet and have samples collected and submitted for testing. “Late intervention, incorrect diagnosis, and inappropriate treatment regimens may lead to poor health and sufferance of patients, which should and can be avoided,” they added.
This case study highlights the importance of consulting a vet any time you suspect a fungal infection and underlines some of the complications that can occur from self-diagnosing horse fungus.
How Do Horses Get Horse Fungus?
Some of the most common fungi, like Ringworm, for example, are highly contagious and can be passed from one animal to another through direct contact, contaminated grooming equipment, and infested stables or trailers.
Environmental conditions can exacerbate both the severity and the spread of a horse’s fungus. Ringworm, for example, is more prevalent during moist, warm weather, while the potentially fatal pythiosis fungal infection is transmitted via contaminated water.
A horse that’s already compromised or suffering from a skin condition other than horse fungus is more susceptible to fungal infection. Similarly, horses on a poor diet or those kept in poorly managed yards or stables are more prone to ringworm than those with a healthy diet and plenty of turn-out time.
Ill-fitting tack can cause friction rubs that can quickly become infected with a horse fungus. Rugs and blankets can retain moisture and hold onto fungus spores for long periods.
Your horse can also acquire some types of horse fungus through ingestion or inhalation. Aspergillosis or Guttural Pouch Mycosis, for instance, is frequently caused by airborne fungal spores. However, if present in your horse’s feed or pasture, the aspergillus fungus can produce mycotoxins associated with Aflatoxin poisoning and equine leukoencephalomalacia.
Preventing Horse Fungus
Different types of horse fungus thrive in various conditions. But, sound habits can help prevent your horse from contracting horse fungus. Keep their stable and pen consistently clean and dry. Change out bedding often, especially during humid months. Wash off sweat after exercise. Give your horse as much time outside in the sun as possible to boost its immune system.
- Ensure your horse is stabled in a clean, dry environment. If you live in a humid area, consider switching from straw to wood or paper-based bedding, which is more absorbent than straw and therefore less likely to create the damp conditions that fungi thrive in.
- Give your horse as much turnout time as possible. Exposure to sun and air will help prevent fungus and aid in the treatment of any superficial infections.
- Consider preventing your horse from accessing ponds or other areas of stagnant water where the fungus spores responsible for pythiosis infections flourish.
- Avoid over-rugging your horse as this can stimulate sweat production, creating a humid environment in which horse fungus can flourish.
- Wash your horse down thoroughly after exercise, taking care to target notoriously sweaty areas. This removes the potential build-up of bacteria that can irritate the skin, making your horse more susceptible to fungal infections.
- A horse on a well-balanced diet complete with beneficial yeasts, pre-and probiotics will have a more robust immune system, making it more able to fight off fungal infections of all types.
- Treat any superficial wounds or scratches with a non-irritating antibacterial cream. This will help accelerate healing, thereby reducing the risk of a fungal infection.
- Make sure your tack fits correctly. Ill-fitting or dirty tack is more likely to rub, putting your horse at greater risk of contracting ringworm and other common types of horse fungus.
Proper stable management and good nutrition can go a long way to preventing horse fungus while keeping your horse’s immune system in optimal condition, making it more capable of fighting infection.
Checking your horse daily for scratches, insect bites, and other skin irritation can also reduce the risk of fungal infection, as can picking out his feet regularly and washing him thoroughly after exercise.
If you notice any lesions or nodules on your horse, contact a vet immediately. This will allow you to get a diagnosis and begin antifungal treatment promptly. The faster it’s treated, the less the fungus will impact your horse’s immune system.
In addition to these precautions, you can limit the possibility of your horse contracting a hoof fungus by soaking his feet in a mild solution of 50% apple cider vinegar and 50% water once a week.
Conclusion
Fortunately, my horse’s hoof fungus shows signs of improvement and appears to be responding well to treatment. However, this isn’t the case with all horse fungus, which is why getting a professional opinion is so vital.
A small lesion on the skin may look harmless enough but could be the start of a potentially life-threatening fungal infection. Even ringworm, which is relatively easy to identify, can only be accurately diagnosed by testing the fungal culture present in a skin biopsy or hair sample.
Not only can early diagnosis and treatment reduce the spread of horse fungus, but it also gives your horse the best chance of making a full and speedy recovery. Despite that, a severe fungal infection could take weeks, if not months, to heal, which is why prevention is a more practical approach.
Resources
- MSD Vet Manuel
- Deep Mycoses
- Anipedia.org
- Bariparasitology. it
- Fungal Infections in Horses
- Fungal Skin Conditions
My Favorite Equine Resources For Horses and Donkeys
This list contains affiliate products. Affiliate products do not cost more but helps to support BestFarmAnimals and our goal to provide farm animal owners with accurate and helpful information.
Squeaky Chicken Toy is hilarious to watch and the horses love it! It’s not super tough so keep it away from dogs.
Dewormer with Ivermectin: I use this for my horses and my goats. Duvet makes a great dewormer. I switch between the Ivermectin one and one like this one so the worms don’t get immune to it.
Manna Pro Apple Flavored Nuggets are a delicious smelling treat that my horses go crazy over.
Equinity Amino Acid Supplement for Horses makes a big difference for any horse that’s struggling with arthritis, hoof issues, or just generally. It’s great for older horses who can’t absorb all the nutrients in their food as well!
Manna Pro Weight Accelerator helps older horses gain weight and stay healthier! This was especially helpful when one of my older horses lost weight over the winter and helped her regain her weight over the summer!
Farnam Fly Control goes on the horse or donkey and will keep the flies off your sweet pet. It makes horses way more comfortable and will keep sores from getting infected as well.
Wound Kote protects sores and wounds. It acts as an antiseptic and helps wounds heal faster. It works on both my horses and goats.

